 Plicae are some of the normal structures of the knee joint cavity Dupont JY. Synovial plicae of the knee. Clin Sports Med. 1997;16(1):87-122. They are folds of the capsule of the joint that surround the patella
(kneecap). The pleats are variable in size and structure between individuals. There
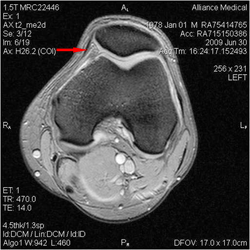
are at least 4 in most knees. The plicae are the "meniscus" of the patellofemoral joint. In this knee MRI the medial plica is indicated by an arrow on the inside of the left knee.
Plicae are some of the normal structures of the knee joint cavity Dupont JY. Synovial plicae of the knee. Clin Sports Med. 1997;16(1):87-122. They are folds of the capsule of the joint that surround the patella
(kneecap). The pleats are variable in size and structure between individuals. There
are at least 4 in most knees. The plicae are the "meniscus" of the patellofemoral joint. In this knee MRI the medial plica is indicated by an arrow on the inside of the left knee.

Совет
о коленной
боли
Здесь пациенты могут найти важную, полезную информацию о проблемах, связанных с коленным суставом.
Г-на
Харди
считают
экспертом в
области
коленной
хирургии,
повреждения
колена,
спортивных
травм,
ортопедии и
травматологии.
В
следующих
разделах
можно найти
информацию
о болезнях
колена,
которые
могут
вызвать
артрит или
коленный
артрит. Г-н
Харди
объясняет,
как
предотвратить
артрит
коленного
сустава.
Нажмите
на картинку,
чтобы
смотреть
видео
операции. Г-н
Харди
работает,
чтобы
предотвратить
остеоартрит.
У
Г-на Харди
есть много
пациентов,
которые
приходят к
нему в
Лондоне из
России.
Если
вам
интересно и
вы хотите
записаться
на приём к Г-ну
Харди в его
клинике в
Лондоне,
пожалуйста,
позвоните
по телефону :
0044 1173171793.
Г-н
Харди
переведёт
всю
информацию
в течение
следующих
нескольких
месяцев с
помощью
русских
коллег.
Пожалуйста,
возвратите
часто, чтобы
проверить
на наличие изменений
Glossary
- Plicae
- Hoffa's Fat Pad
- Arthroscopy
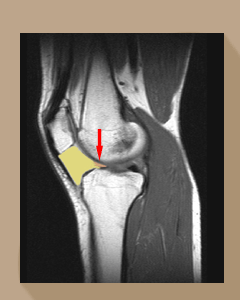 The anatomy of the fat pad has been well described anatomically Gallagher J, Tierney P, Murray P, O'Brien M and radiologically Saddik D, McNally EG.
The anatomy of the fat pad has been well described anatomically Gallagher J, Tierney P, Murray P, O'Brien M and radiologically Saddik D, McNally EG.
The red arrow points to the tongue of the fat pad (yellow) that catches between the condyle of the femur and the tibia. The condition, from chronic impingement then scarring of the fat pad, was first reported by German surgeon Albert Hoffa in 1904 (Albert Hoffa, 1859-1907) so it is odd that it has taken so long to recognise it as a common and genuine condition in athletes. Emad Y and Ragab Y.
The Hoffa's fat pad is known to be richly innervated with sensory fibres Wojtys EM, Beaman DN, Glover RA, Janda D. Innervation of the human knee joint by substance-P fibers. Arthroscopy 1990;6(4):254-63.
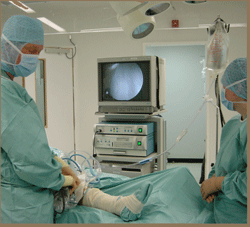
Arthroscopy of the knee is an operation on a joint which is done by a minimally invasive technique.
A narrow lens, on the back of which is a video camera, is inserted into the joint to allow examination of the inside.
By using specially designed probes and instruments, the surgeon can also do some treatments to the inside of the knee joint.
Why should it be done? It would only be done if you have persistent symptoms from your knee such as pain, locking, swelling or giving way. These symptoms are indicative of ongoing impingement and wear in the knee. Look at the video to the right of a lateral meniscal tear missed by an MRI scan. There has been little wear and tear of the surface of the joint from the hard gristle of the unstable meniscal tear because it was dealt with promptly by keyhole surgery. Compare it to the arthroscopy video above it where time has elapsed between onset and treatment. It is easy to see why a neglected or missed meniscal tear is the most common cause of unicompartmental osteoarthritis.
Arthroscopy of the knee is usually done after an injury which is failing to settle at 6 weeks with conservative treatments such as RICE, knee supports and physiotherapy and where there is evidence of damage to the ligaments, cartilages, lining or surfaces of the knee joint. If it is done for an injury, a MRI scan of the knee will be done first to alert the surgeon to what may be found inside the joint before the procedure so that he can properly advise on the prognosis. Read this file if Mr Hardy has offered you an arthroscopy of the knee...
The protocol to the left is for a W8200 - Arthroscopy and Partial Menesectomy.
The protocol to the right is for a W8200, W8300 - Arthroscopy, Partial Menesectomy and Chondroplasty.
The protocol to the left is for a W8230 - Arthroscopy and Meniscal Repair.
The protocol to the right is for a W7420 - Arthroscopic ACL Reconstruction.
The protocol to the left is for a W8150, W3110, - Arthrotomy, Mosaicplasty and chondral fixation..
Knee Problems
Plica Syndrome
A tear of one of the plicae can result in the pain of impingement which is worse climbing or descending stairs.The least common is the lateral patella plica. The most common is the medial patella plica. The medial and lateral patella plicae have a load sharing function for the patella and trochlea (kneecap and thigh bone) in much the same way as the menisci (cartilages) are for the tibio-femoral joint (thigh bone and shin bone). The suprapatella plica, medial plica and infrapatella plica are not without clinical relevance. The plicae are associated with an age related development of osteoarthritis Lyu & Hsu 2006.
The relief of pain and prevention of progression of osteoarthritis is the main benefit of conservative treatments using physiotherapy, McConnell taping, and knee patella braces and supports.
Occasionally minor day case keyhole surgery is needed. The results are very successful for plica syndrome before grade 3 degenerate change of the cartilage has taken place Gerbino PG 2nd, Micheli LJ. Bucket-handle tear of the medial plica. Clin J Sport Med. 1996 Oct;6(4):265-8; discussion 268-9. and O'Dwyer KJ and Peace PK. Injury. The plica syndrome 1988;19(5):350-2.
The video demonstrates reversal of degenerate change on the patella 18 months after a suprapatella plica and the very small scarred portion of Hoffa's fat pad have been removed...
The video below shows the impingement of the scarred medial plica between the kneecap (patella) and the trochlea of the thighbone (femur).
The damage to the hyaline cartilage surface seen above causes crunching when going up and down stairs and getting out of a chair (crepitus).
Crepitus with pain requires referral for assessment in order to prevent osteoarthritis of the knee...
The complete suprapatella plica causes knee pain in long distance cyclists and runners. The day case keyhole surgery is relatively simple with minimal pain and patients walk home the same day crutch free...
Most patients with persistent knee pain would go to a doctor. Patients with persistent knee pain above the knee and a swelling would usually get this sorted out quite quickly. This is a video of a patient with persistent pain and swelling above the knee who was told by another Consultant Orthopaedic Surgeon that nothing could be done for her. She struggled on for 2 years until she decided to pay for private treatment. The knee was cured with a 20 minute arthroscopy using the new Arthrocare Ambient radiofrequency technology.Have a look at the new technology in the video below...
The incomplete suprapatella plica often cause the patient to feel intermittent tugging pain above the knee cap on the inside or outside of the knee. In some circunstances it contributes to higher than normal pressures in the patellofemoral joint that can be relieved by this procedure...
Some patients tear the plica like they tear a meniscus. This torn plica forms a band which rubs across the hyaline cartilage of the femur causing pain, degenerate change and eventually osteoarthritis. It is often difficult to spot on an MRI scan which is why if the symptoms and clinical signs suggest this diagnosis Mr Hardy reviews the MRI scan personally .
The infrapatella plica is usually known as the “ligamentum mucosum”. It lies just behind the lower pole of the patella. The plica is intact in early life and may or may not be present in the elderly implying in some patients lifetime it has ruptured. A torn infrapatella plica can cause symptoms of knee pain going up stairs. It lies in the same plane as the anterior cruciate ligament. This suggests that the same type, but not necessarily magnitude, of injury that ruptures the ACL also ruptures the infrapatella plica Abreu MR et al. Hoffa's fat pad injuries and their relationship with anterior cruciate ligament tears. Skeletal Radiol. 2008;37(4):301-6.
The infrapatella plica can be considered equivalent to a washing line that supports the Hoffa’s infrapatella fat pad. Tear of the infrapatella plica is not without clinical relevance when it intermittently gets caught beneath the knee cap causing pain and if consistent degenerate change leading to arthritis.
The relief of pain and prevention of progression of osteoarthritis is the main benefit of both conservative management using physiotherapy and knee patella braces and supports or keyhole surgery for this condition...
Click on the icon below for the talk Mr Hardy prepared for colleagues on this subject It is best viewed after his lecture as a memory aid...
Painful Bands in the Knee
An intra-articular band of the knee is often easy for the patient to localise (a clinical symptom) but rarely are there clinical signs of this painful condition. The MRI scan is usually normal. However, take a careful history in these patients and the condition can be demonstrated and cured easily with day case keyhole surgery.
Patients can often point exactly to the place where the torn band from the plica is attached. There are other causes of intra-articular (in the joint) bands...
An adhesion is an intraarticular band that has formed after a bleed into a joint. Adhesions form from the organisation of the blod clot that forms in a joint after injury or surgery. This happens in joints in much the same way as adhesions form in the abdominal cavity.
The incidence of adhesions after arthroscopic surgery of the knee can be reduced by careful control of haemostasis during surgery by using the correct instruments. The effects of adhesions can be mitigated by the correct postoperative rehabilitation. The video below explains how surgeons like Mr Hardy use modern technology to stop bleeding...
Hoffas Fat Pad Impingement
Hoffa's Posterior Fat Pad Impingement (HPFPI) syndrome is no longer as rare as first thought Krebs VE and Parker RD.
Mr Hardy's analysis of his arthroscopic experience since January 2001 is that on its own it accounts for approximately 12% of anterior knee pain. His analysis also shows it is associated with meniscal tears in nearly 25% of all patients undergoing arthroscopy for this condition. The treatment for this condition was described in the scientific literature 18 years ago Magi M, Branca A, Bucca C, Langerame V.
Hoffa's Fat Pad Impingement affects either the top or the bottom of the fat pad and occasionally both (apparent in patients who still have pain after keyhole surgery where only one has been addressed by the surgeon). The keyhole surgery for this condition requires special expertise and approach which is why it is often missed on the routine knee arthroscopy leaving patients with unexplained pain following arthroscopy (Morini G et al)
Below is a clip of a patient with inferior posterior Hoffa's impingement and early degenerate change of the articular cartilage...

The relief of pain and prevention of progression of osteoarthritis is the main benefit of both conservative management using physiotherapy, patella taping patella braces, patella straps and knee supports.
It is Mr Hardy's experience that a third of the patients he has assessed can be cured with patella taping (similar to that employed by Rafael Nadal) and physiotherapy.

Some patients do not respond to patella taping and these require a simple day case procedure. Anterior Knee Pain from conditions like Hoffa's is becoming much easier to treat with the advances in understanding and the better equipment available. Read about the experience of just one of Mr Hardy's patients who works for the French Insurance Company AXA. He now has a pain-free kneecap.
Meniscal Tear
Hoffa's fat pad impingement appears to be 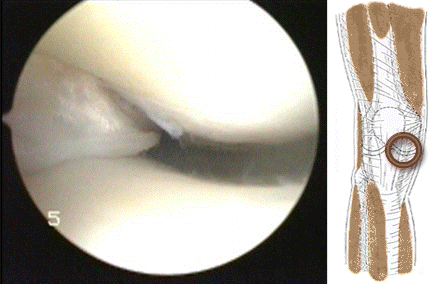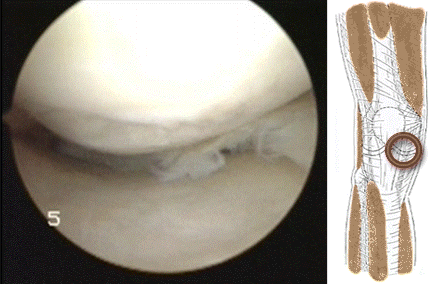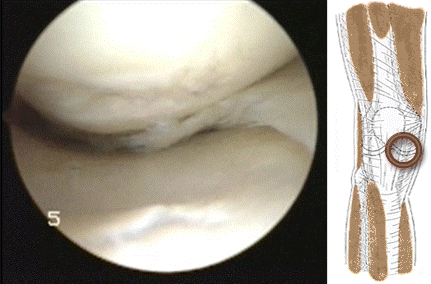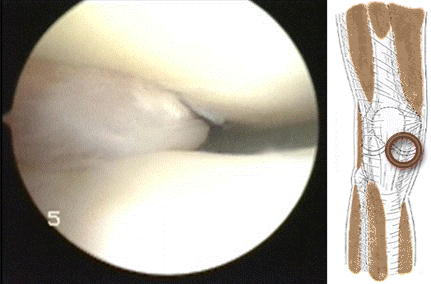 frequently associated with meniscal tearing. It might be that impingement at the front of the knee causes a shearing force on the meniscus at the back of the knee resulting in a tear of the meniscus as in the video above.
frequently associated with meniscal tearing. It might be that impingement at the front of the knee causes a shearing force on the meniscus at the back of the knee resulting in a tear of the meniscus as in the video above. 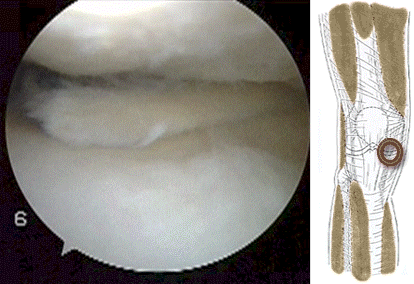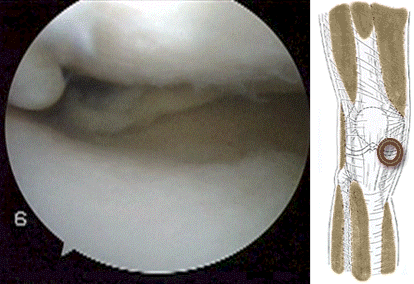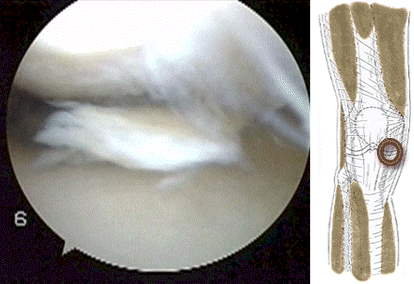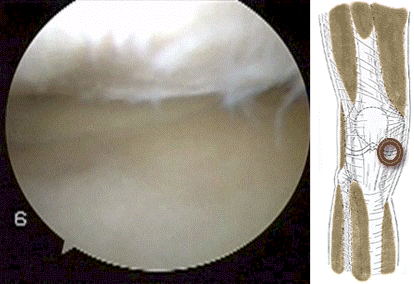 The meniscus can tear more than once as shown by the video below of a patient with a second meniscal tear of the lateral meniscus treated during ACL reconstruction...
The meniscus can tear more than once as shown by the video below of a patient with a second meniscal tear of the lateral meniscus treated during ACL reconstruction...
There are two causes and two types of meniscal tear.
Meniscal tears can be traumatic or degenerative. The traumatic type are associated with an obvious history of injury. The degenerative type are not associated with a history of injury (Drosos GI, Pozo JL. The causes and mechanisms of meniscal injuries in the sporting and non-sporting environment in an unselected population. Knee. 2004;11(2):143-9.).
Meniscal tears can be asymptomatic and stable or symptomatic and unstable (Zanetti M, Pfirrmann CW, Schmid MR, Romero J, Seifert B, Hodler J. Patients with suspected meniscal tears: prevalence of abnormalities seen on MRI of 100 symptomatic and 100 contralateral asymptomatic knees. AJR Am J Roentgenol. 2003 Sep;181(3):635-41.).
Unstable meniscal tears cause osteoarthritis (Suter LG, Fraenkel L, Losina E, Katz JN, Gomoll AH, Paltiel AD. Medical decision making in patients with knee pain, meniscal tear, and osteoarthritis. Arthritis Rheum. 2009 Nov 15;61(11):1531-8.).
Osteoarthritis causes both stable and unstable meniscal tears. Englund M, Guermazi A, Lohmander SL. The role of the meniscus in knee osteoarthritis: a cause or consequence? Radiol Clin North Am. 2009 Jul;47(4):703-12.
If you have an unstable meniscal tear and have been advised by your surgeon that you need keyhole surgery read this information sheet about knee arthroscopy...
ACL Tear
 This is a copy of the patient information sheet for ACL reconstruction and rehabilitation.
This is a copy of the patient information sheet for ACL reconstruction and rehabilitation.
Knee ACL reconstruction is highly successful these days. However, about 50% of all athletes that rupture their ACL do not require surgery but rehabilitation and an ACL Brace. In the patient not requiring surgery rehabilitation is as important, if not more so, than the athlete who does want surgery to stabilise their knee.
Anterior Cruciate Ligament surgery and rehabilitation have undergone dramatic changes recently. This is due to scientific research, improved surgical technique, extensive clinical experience and better understanding of the consequences of rehabilitation. ACL Surgery prevents instability that might cause meniscal tear. Meniscal tears, when unstable, are a potent cause of arthritis. Therefore, a priori, ACL reconstruction prevents arthritis....
Recent advances have led to the use of calcium composite screws in ACL reconstruction that are replaced over the years with bone. This has advantages to professional and amateur athletes as discussed in this video...
Mr Hardy recommends Accelerated Rehabilitation after ACL reconstruction. He recommends a Knee Sleeve for activities in the first two years after surgery and an ACL Knee Ligament Brace for skiing, water skiing etc.
Synovial Chondromatosis
Synovial chondromatosis is a complex problem that can be resloved by any accomplished arthroscopist if a basic understanding of the causes is appreciated. Mr Hardy has experience of management of this condition to cure it by day case keyhole surgery. Click on the pdf file above for more information and the video below to understand the treatment...
Pigmented Villonodular Synovitis (PVNS)
Pigmented villonodular synovitis (PVNS) is a disease in which the tissue lining the joints and tendons in the body (synovium) grows abnormally. It is a noncancerous tumor but it is locally agressive. It is not common but the knee is most commonly invloved. There are two types of PVNS: the local or nodular form (where the tumor is a localised swelling) and the diffuse form (where the entire lining of the joint is involved). Symptoms include pain, swelling with limitation of range of movement and locking of the joint. The average age of diagnosis for this condition is 35 years. The cause of PVNS is unknown. Treatment involves surgery to remove the tumor and damaged portions of the synovium.Click on the video below to see the latest techniques to deal with the nodular type of PVNS through minimal keyhole surgery and same day return to walking...
Bipartite Patella
This is an acquired condition of childhood. It is one of the overuse injuries that happen through excessive and sustained sporting activity in children. Athletes are never born with a bipartite patella as is claimed for Andy Murray.. This is a common misconception. A bipartite patella can be seen in up to 2% of the population. Click on the icon below to read more....